SURGERY
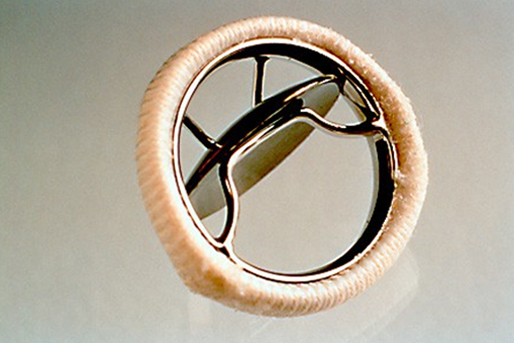
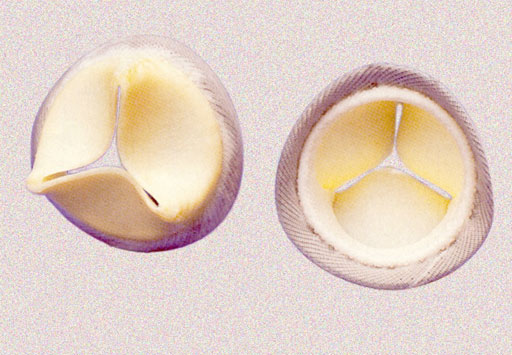
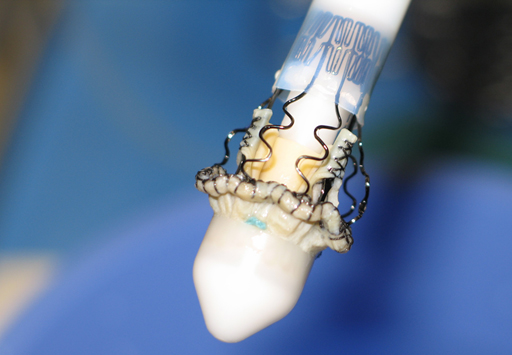
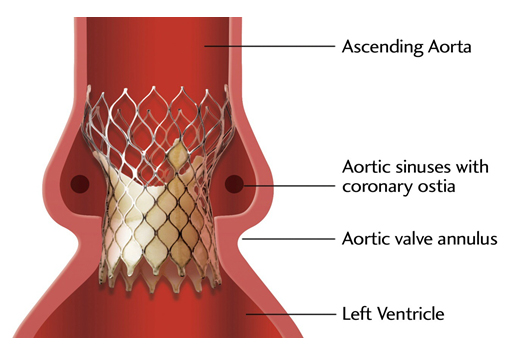
Edwards Sapiens and Corevalve valve.
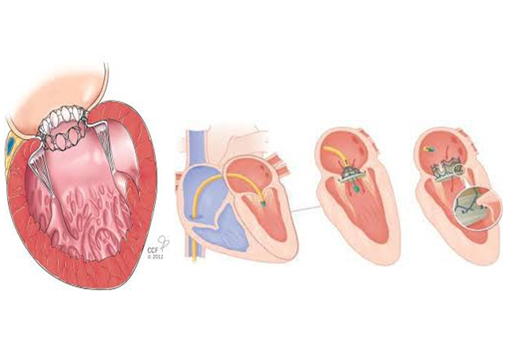
A innovative surgical approach has been adopted in recent decades with implantation of aortic valves correlated with techniques of endovascular catheterisation.
The introduction of these so-called peri-cutaneous valves into surgery provides new models of prostheses using new means of attachment and based on the principle of stent placement with a memory of shape.
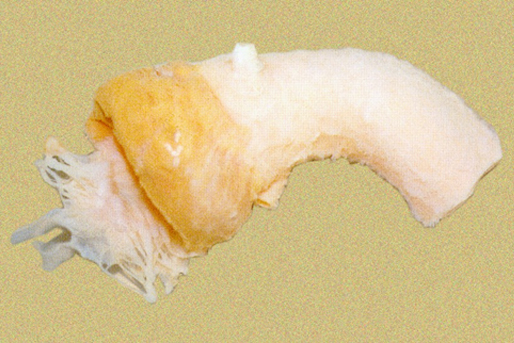
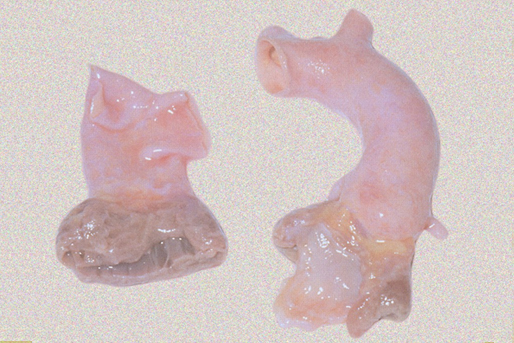
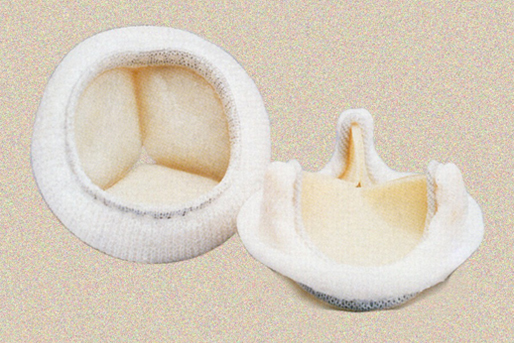
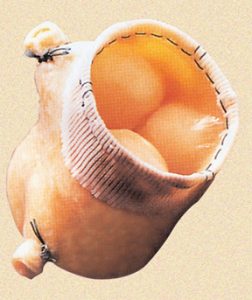
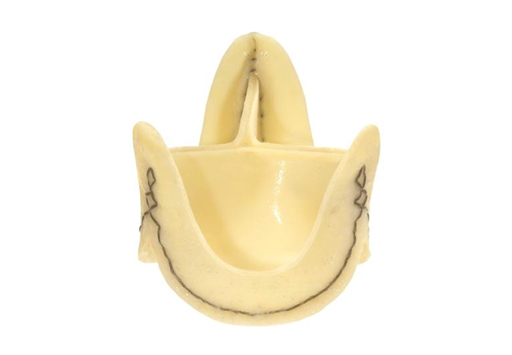
The Sorin Solo valve (Sorin Solo stentless valve, without a support medium)
generally is implanted on the wall of the aorta with a single line of sutures.
Surgical replacement of the aortic and the mitral valves by mini-thoracotomies improves the patient’s quality of life. They mean we can avoid a complete median sternotomy and reduce surgical trauma by decreasing the size of the incision and facilitate post-surgical follow-up. The combination of a mini sternotomy and of a sutureless valvular prosthesis (without sutures) and of its rapid deployment have provided a true gain in time and simplification of open-heart conventional aortic valvular surgery. The major advantage of this technique compared to TAVI is the possibility of excision of a calcified valve, thus enabling complete deployment of the prothesis.
The second advantage of this simplified technique is to treat coronary or other valvular lesions.
It is therefore possible to perform aortic implantations in 20 minutes as opposed to up to 50 minutes. The combined use of a sutureless prosthesis with CABG[1] on a beating heart with ECC (Pump Off) enables us to perform an impressive procedure, in the elderly, 2 to 3 CABG on a beating heart together with aortic valve replacement in about only 20 minutes of ECC and clamping of the aorta.
Therefore, the post-surgical follow-up is less complicated in terms of pain, major blood loss and risk of transfusion and also duration of hospital stay is shortened. Convalescence is reduced, the patient can resume his or her activities more quickly. And without mentioning the improved cosmetic presentation!
[1] CABG: Coronary artery bypass grafting